Mental Health Strategy for Scotland: 2012-2015
The Scottish Government’s mental health strategy to 2015 sets out a range of key commitments across the full spectrum of mental health improvement, services and recovery to ensure delivery of effective, quality care and treatment for people with a mental illness, their carers and families.
This document is part of a collection
Key Change Area 1: Child and Adolescent Mental Health
Infant and Early Years Mental Health
"The period between pregnancy and 3 years is increasingly seen as a critical period in shaping children's life chances, based on evidence of brain formation, communication and language development, and the impact of relationships formed during this period on mental health. It is therefore also a critical opportunity to intervene to break cycles of poor outcomes."41
The Scottish Government is already committed to publishing a Parenting Strategy later in 2012 with a focus on work to support parents to be competent and confident in their efforts to build strong attachments with babies and young children. This will build on existing policy and on the day to day activities of midwives, public health nurses, nursery teachers and others. The Scottish Government is also committed to an expansion of the Family Nurse Partnership42 - a model of delivering intensive support to vulnerable young first time mothers which has been shown to significantly improve a range of outcomes for children. We are already working through the Early Years Taskforce to prioritise and invest in interventions for which there is sound evidence of effectiveness.
However, we know that there is more that could be done for those who are most vulnerable. Secure attachment and competent, confident parenting are known to be significant protective factors, conferring confidence, resilience and adaptability. Disorganised attachment in infancy has been linked by both longitudinal and retrospective studies to a number of severe mental health problems manifesting in later life43. The importance of early experience in creating the conditions for good or poor mental health cannot be overstated.
Those most in need of help can be either easy or hard to identify depending upon whether the manifesting problems are visible (e.g. young children with very challenging behaviour) or hidden (e.g. babies who may be quietly suffering and anxious because their needs for social interaction through secure attachments are not being met).
Responding Better to Conduct Disorders
It is normal for young children to display challenging behaviour by being non-co-operative, highly emotional and aggressive, at times. Generally, these behaviours peak in the early pre-school years and start to reduce by the time children start school. However, approximately 10% of young children show a different developmental pattern44. For these children, their already elevated levels of aggression, non-compliance and emotional distress persist throughout childhood. As the diagram below shows, for many, the pattern endures into, and throughout, adulthood45.
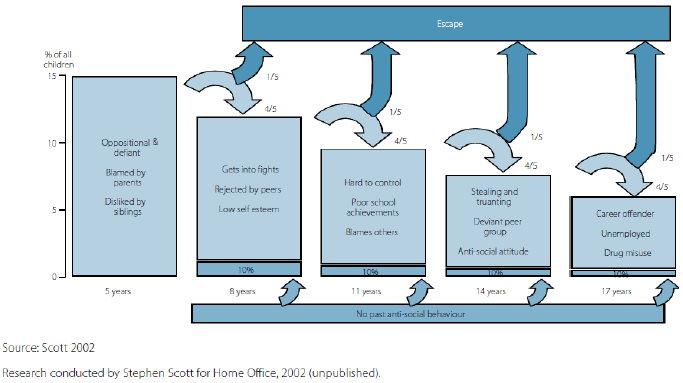
The reasons for these behaviours are complex, but we know that this pattern of behaviour problems is a powerful indicator of risk of long-term negative personal and social outcomes, including school disruption, family stress and dysfunction, mental health problems, loss of employment productivity, social isolation, drug and alcohol problems, as well as crime and antisocial behaviour46. A longitudinal study showed that antisocial behaviour at age 13 was predicted by externalising behaviour at age three47. Another study showed that by age 28 those with conduct disorder in childhood were 3 times more likely to have been convicted of a crime than those with no problems (and 12 times more likely to have spent time in prison)48.
Evidence-based parenting programmes, such as Triple P and Incredible Years, offer a powerful way of addressing and responding to these early-onset behaviour problems. They are relatively inexpensive and produce long term benefits to the individual and society. The programmes take a positive and assets based approach to strengthening parental competencies. For those with early onset disruptive behaviour problems there is over 30 years worth of top quality research demonstrating the effectiveness of parenting programmes based on social learning theory. The research shows that, after their parents had participated in one of these group-based parenting programmes, roughly two-thirds of the children (with early onset disruptive behaviour) were behaving at a level comparable to that of their peers49. Research results have been replicated in randomised control trials by independent research teams in various countries worldwide as well as in Britain50.
A partnership between the NHS and Glasgow City Council is in the process of making Triple P available to all parents in the city of Glasgow. Hundreds of practitioners, including health visitors, social workers and nurses, have already been trained to deliver the programmes. We believe that we should build on this approach and that a nationally coordinated approach is the best way of maximizing efficiencies and ensuring the quality of training and supervision, thereby ensuring that the programmes are delivered in accordance with the research evidence.
Commitment 7: In 2012 we will begin the process of a national roll out of Triple P and Incredible Years Parenting programmes to the parents of all 3-4 year olds with severely disruptive behaviour. We will include more information about the delivery of this commitment in our Parenting Strategy which will be published in October 2012.
Responding Better to Attachment Issues
Secure attachment is a basic human need of all infants but not one which is always met. An infant whose attachment becomes disorganised can experience high levels of stress and anxiety without necessarily showing outward displays of distress which would signify to their caregiver or the other adults in their support system that something is wrong.
We know about the importance of attachment and we also know a bit about what interventions are effective to address attachment issues in individual cases. Where the key challenge lies is in designing and developing good systems which combine raised levels of general awareness, a capacity to identify enhanced need and a capacity to respond appropriately and effectively when enhanced need has been identified. In order to address this 'hidden' health need of the present and improve the mental health and wellbeing of our future population we need to do three things. We need to do more to improve the general understanding of the issue of attachment, we need to improve the skills and awareness of those who come into contact with infants so that attachment problems or potential problems are recognised and where possible addressed, and we need to improve access to specialist support such as parent infant psychotherapy where this is indicated as necessary.
We are committed to gaining a better understanding of how the range of elements, outlined above, fit together to make up a good infant mental health service system. To do this we intend to examine the range of services and models of delivery currently in operation in Scotland and elsewhere and to learn from the latest available evidence about what systems are effective. We shall also focus attention on specific areas of innovative practice - for example following, with interest, the progress of the New Orleans Intervention model - being delivered and evaluated in Glasgow by NSPCC in partnership with Glasgow City Council and NHS Greater Glasgow and Clyde. The New Orleans Intervention Model was developed in the USA and is a cutting edge way of intervening with abused and neglected pre-school children51. This is a potential prototype for a new way of working nationally.
Commitment 8: We shall make basic infant mental health training more widely available to professionals in the children's services workforce. We shall also improve access to child psychotherapy (a profession which specialises in parent infant therapeutic work) by investing in a new cohort of trainees to start in 2013.
Looked after Children
Research carried out in the UK and elsewhere consistently shows that looked after children have significantly poorer mental health than the rest of the population52. Work with this particular group is often made more complex by the strong feelings which can be evoked in care-givers and professionals by children who are struggling to cope with and come to terms with a personal history of trauma including abuse and neglect.
In recent years there have been many positive developments, both in relation to an increase in direct therapeutic services for this population and an increase in the indirect mental health support available. An example of the indirect support is the basic mental health training which has been made available to all those working with or caring for looked after children and young people53. In addition, NHS Boards are required to assess the mental health needs of all looked after children for whom they have a responsibility54.
There is still work to do to improve the way in which Child and Adolescent Mental Health (CAMH) services, local authorities and third sector providers work together to address the mental health needs of this population. Services work best for children where NHS Boards are able to deliver training and also opportunities for professionals to discuss particular concerns about an individual child or young person in care, where work has been done to develop a shared understanding of thresholds (the signs and symptoms of distress and/or mental illness which make a specialist CAMHS assessment or intervention necessary), where good professional relationships between individuals from different agencies have been allowed to build up over time, and where there is confidence that new referrals for assessment will be given appropriate priority. In accordance with Getting it Right for Every Child principles we shall continue to encourage high quality, individually tailored, multi agency approaches for this vulnerable group55.
Commitment 9: We will work with a range of stakeholders to develop the current specialist CAMHS balanced scorecard to pick up all specialist mental health consultation and referral activity relating to looked after children.
Learning Disability and CAMHS
We know that access to mental health services for children with a learning disability is better in some parts of Scotland than in others. This work is complex and challenging, with combinations of learning and developmental disorders as well as mental illnesses giving rise to a wide range of presentations, uncertainties about diagnosis and difficulties in identifying effective treatment regimes which are sustainable over time. Different approaches to service delivery are also taken in different parts of Scotland. We have recently produced a report to support service development which will be made available and issued to NHS Boards and we will work with clinicians to take forward key actions identified from the report.
We are collecting data, through the CAMHS Balanced Scorecard, on the numbers of children with learning disability gaining access to mental health services in different parts of the country. This will help us towards a better understanding of the variance and help NHS Boards to take appropriate action, where necessary, to improve access in the short term.
Commitment 10: We will work with clinicians in Scotland to identify good models of Learning Disability CAMH service delivery in use in different areas of Scotland or other parts of the UK which could become or lead to prototypes for future testing and evaluation.
Access to Specialist Child and Adolescent Mental Health Services
Much work has been undertaken nationally over the past 3 years to improve access to specialist CAMHS by reducing the time patients wait between referral and treatment. This followed the setting of a HEAT target which states "no patient shall wait longer than 26 weeks between referral and treatment for specialist CAMHS by March 2013". An additional target of 18 weeks by December 2014 has now been set to bring the target into line with other access time targets and the access to psychological therapies target.
We are on track to deliver the HEAT target, reflecting a significant service improvement and reduction in waiting times. Data suggests a reduction from over 1200 waits of over 26 weeks when we began this work to around 300 currently and with further work in hand that will assure delivery of the target. The target is intended to reduce waiting times and improve access to CAMH services overall, but it does not remove the role of clinicians in deciding when a child needs to access a service more quickly. Where a child or young person is assessed as needing to access a service urgently, they will be seen more quickly, sometimes the same day.
Changes have been achieved in a number of ways. Firstly there has been a focus on growing the specialist CAMHS workforce which has increased by over 34% in less than four years from 645.3 whole time equivalents (WTE) in September 2008 to 868.9 WTE in March 2012 (see graph below). We have worked on capturing data to measure CAMHS waits which is due to be published for the first time in August 2012 by ISD. There has also been a significant amount of service and patient pathway redesign work undertaken which has ensured a more efficient and effective use of resources.
The growth in the total whole time equivalent (WTE) for the CAMHS workforce, September 2008 through to March 2012 is shown in the graph below.
Total CAMHS workforce
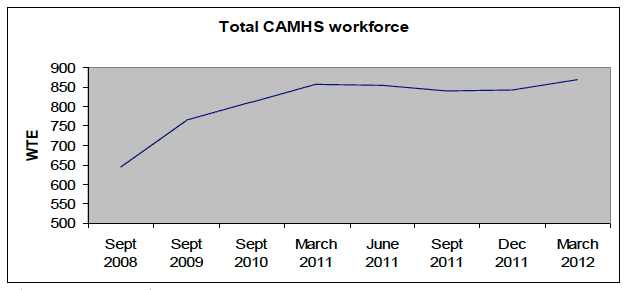
Note: Numbers exclude trainees
Source: Child and Adolescent Mental Health Service Workforce Database.
Commitment 11: We will work with NHS Boards to ensure that progress is maintained to ensure that we achieve both the 2013 (26 week) and the 2014 (18 week) access to CAMHS targets.
CAMHS Admissions to Adult Beds
A decision to admit a young person to an adolescent unit will be made only if admission is deemed the only safe and appropriate option available for the patient. It is important therefore that beds are available when required. In order to ensure that this is the case two approaches are being taken nationally. Firstly a decision of the North of Scotland NHS Boards to build a new 12 bedded unit in Dundee to replace the current 6 bedded unit will increase the bed base from 42 to 48 beds and improve the quality of the estate. Secondly a new model of care and treatment has been introduced. This new approach to addressing the issue of capacity has seen the development of CAMHS intensive 'hospital at home' type service delivery in a number of NHS Board areas.
The new approach used emphasises the child's strengths and uses the expertise within the family and the local community to maximise the support available - the theory being that a small change in a child's familiar environment will be more significant in their recovery than a larger change in a setting alien to them. When provided in conjunction with practices such as proactive discharge (planning discharges from the date of decision to admit) and flexible approaches to in-reach and out-reach work, a number of benefits have been demonstrated. Some admissions are avoided altogether. Many are significantly shortened. Where evaluation and research has been undertaken, good patient outcomes have been demonstrated56.
The benefit to the system as a whole is that new capacity is created. In the areas where the new approaches are most advanced this has been demonstrated to have had the effect of significantly reducing the need for unscheduled and temporary admissions of under 18s to adult psychiatric hospital beds.
Table to demonstrate regional variance in under 18 admissions to adult wards (AWA) and to specialist CAMHS units (SCA) April - Sept 2011
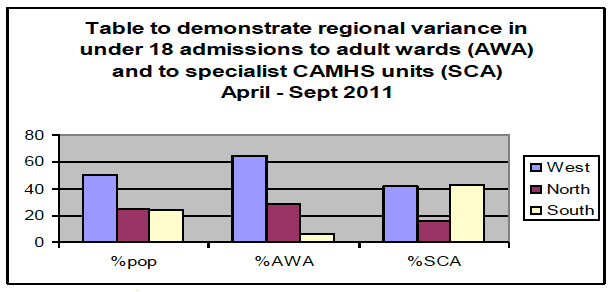
Source ISD SMR04 returns
Focusing on the South of Scotland demonstrates the variance and the potential benefits of newly created capacity, arising from the new model. In a recent 6 month period it was shown that the South of Scotland had 25% of the population but only 5% of admissions to adult wards. During the same period almost half of all admissions to CAMHS specialist units occurred in the South, though this is also the product of shorter admissions, increasing the number of young people accessing the service as is shown in the following graph.
South of Scotland Lothian CAMHS Inpatient Unit
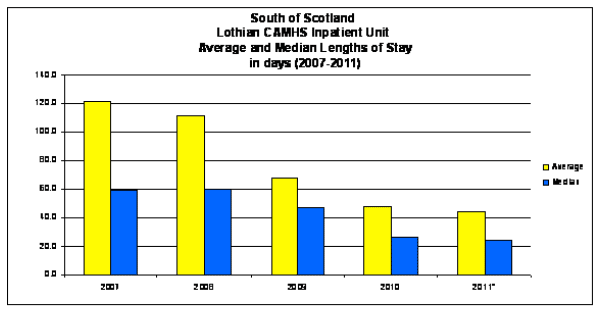
Source NHS Lothian PIMS
This graph shows a dramatic reduction in lengths of stay during the five year period 2007- 2011. While there have been changes elsewhere in Scotland, they have been less dramatic and we will be undertaking further work focused on variance, with the objective of delivering similar benefits to those which have been delivered in the South and East of Scotland Regional Planning Area.
A small number of young people in Scotland with very complex needs are admitted to adult forensic services or specialist services in England. As use of the CAMHS inpatient estate continues to developed, we will consider how the varied and complex needs of this group of young people can best be met.
Commitment 12: In addition to tracking variance and shorter lengths of stay, we will focus on reducing admissions of under 18s to adult wards, with a new commitment to reduce figures across Scotland to a figure linked to current performance in the South of Scotland area.
Child and Adolescent Mental Health Indicators
A set of national mental health indicators for children and young people in Scotland has been established. This complements the mental health indicator set for adults. It was launched formally by NHS Health Scotland in November 2011, with a follow up web publication57. The children and young people's mental health indicators cover both the state of mental health (mental wellbeing and mental health problems) and the associated contextual factors.
The indicators provide for the first time a means of assessing and monitoring the mental health of Scotland's children and young people over time and will enable the development of the first national mental health profile for children and young people (aged from pre-birth to 17 years). Updated every four years, the profile will result in a greater understanding of the current and changing picture of mental health within this population and the factors that influence it.
Contact
Email: Ewen Cameron, Reshaping Care & Mental Health Division
There is a problem
Thanks for your feedback