Better Heart Disease and Stroke Care Action Plan
Revised strategy for heart disease and stroke in Scotland.
2: PROGRESS SINCE 2004
Cardiovascular Disease Mortality
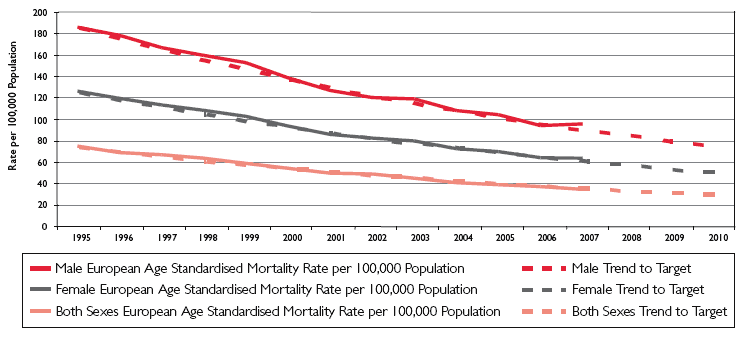
2.1 Across Scotland, all sectors of society have seen over the past decade a continuing and welcome downward trend in cardiovascular mortality, and the gap in mortality between the least and most deprived has narrowed. Graphs 1 and 2 illustrate progress towards the targets of a 60% reduction in premature (<75) CHD mortality and 50% reduction in premature mortality from Stroke between 1995 and 2010 (see graphs below). A further target was set in 2004, aimed at achieving an additional 27% reduction in premature mortality from CHD by 2008 for the most disadvantaged communities. The <75 CHD mortality rate in these communities has decreased by 17% from 135 per 100,000 population in 2003 to 112 in 2007. If this trend continues, the 2008 target should be met. In 2007 this target was superseded by one aiming to reduce CHD mortality among the <75s in the most deprived 15% of areas in Scotland, using 2006 data as the baseline.
2.2 Although excellent progress continues to be made in terms of overall mortality reductions, it is a matter of concern that rates of decline in CHD mortality for men and women aged 35-54 years show recent, significant flattening. Specifically, the annual percentage change in men was - 6.28% between 1986 and 2003, but only - 0.55% between 2003 and 206. Furthermore, a small increase in mortality rates occurred in young men in 2005-06. Between 2003 and 2006 the two most deprived quintiles showed an increase of 16.8% and 10% respectively. This will clearly make the additional 15% mortality reduction target for the most disadvantaged groups more difficult to achieve. These adverse trends mirror what is happening in other parts of the world, including the US and England and Wales. It is clear that unfavourable trends in cardiovascular risk factors (for example, obesity and diabetes) are affecting CHD mortality trends in younger age groups. CHD prevention in younger people needs to be prioritised if the favourable reduction in mortality seen over so many decades in Scotland is to be maintained. This issue is explored in detail in the next chapter.
Graph 1: Coronary Heart Disease; Ages Under 75; European Standardised Mortality Rates per 100,000 Population
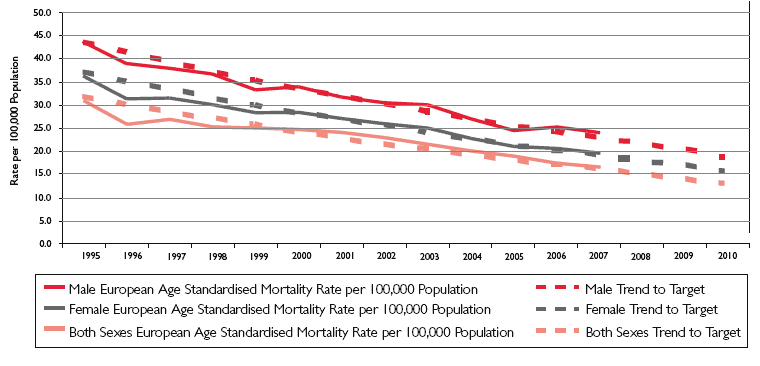
2.3 The trend in terms of stroke deaths is more consistent. The latest figures show a reduction in mortality from stroke in the <75s from 37.5 deaths per 100,000 in 1995 to 18.8 deaths per 100,000 in 2007. If this trend continues, the 50% target reduction in mortality from cerebrovascular disease in this age group should be met. However, it needs to be borne in mind that current demographic trends will result in an increase in the number of patients suffering a stroke, if the age specific incidence is not reduced by primary prevention. Future increases in stroke incidence may also be related to obesity, diabetes and alcohol misuse.
Graph 2: Cerebrovascular Disease; Ages Under 75; European Age Standardised Mortality Rates per 100,000 Population
Service Developments
2.4 The five years since the last Strategy update have seen significant service improvements for both heart disease and stroke. For example, Managed Clinical Networks are now well established in all NHS Board areas, and are being used increasingly as a source of expert advice in terms of service planning.
2.5 In 2007, comprehensive new SIGN Guidelines for CHD and Cardiovascular Disease were published, which include the development of the risk calculator, ASSIGN. The corresponding stroke Guideline was also revised in December 2008.
2.6'Keep Well' services delivering inequalities-targeted health checks for those most at risk of preventable CVD are well established in primary care across Scotland, and continue to be refined to new 'at risk' populations. This is reflected in targets in the National Performance Framework and HEAT.
2.7 Waiting times for investigation and treatment of heart disease continue to fall, with cardiology blazing a trail in terms of progress towards achieving the 2011 target of a maximum waiting time of 18 weeks from referral to treatment for all conditions.
2.8 The Quality and Outcomes Framework ( QOF) of the new General Medical Services ( GMS) contract for primary care from April 2009 includes 134 indicators, covering 20 clinical areas, of which 10 relate to cardiovascular disease: Coronary Heart Disease; primary prevention of CVD; heart failure; stroke/ TIA; hypertension; diabetes; Chronic kidney disease; atrial fibrillation; obesity; and smoking.
2.9 Scottish practice achievement against these indicators in 2007-08 was in the main above 99%, more than the average overall achievement of 98.21% for all indicators. The QOF data demonstrate consistently high achievements in the clinical domains of secondary prevention in CHD and stroke and transient ischaemic attacks, showing that general practice is delivering high quality care for people with these conditions.
2.10 In relation to CHD, technical advances such as drug eluting stents and cardiac resynchronisation therapy have been rolled out across the country by the Regional Planning Groups ( RPGs). The Lothian pilot of primary PCI (percutaneous coronary intervention) has been completed successfully, and RPGs in conjunction with the Scottish Ambulance Service are considering how to implement its findings in other parts of the country. The National Centre for Treatment of Advanced Heart Failure is now well established at the Golden Jubilee National Hospital, and there has been significant progress towards the development of an electronic patient record for cardiology.
2.11 In relation to stroke, access to all-important stroke unit care has improved, with a significant rise in the number of units and designated stroke beds. The Scottish Stroke Care Audit ( SSCA) ( www.strokeaudit.scot.nhs.uk) demonstrates year on year improvements in the elements of stroke care, as measured against NHSQIS standards. As in the case of heart disease, good progress is being made in moving towards an electronic patient record for stroke (see paragraph 7.22 et seq.).
2.12 A number of important educational initiatives led by NHS Education for Scotland ( NES) are also contributing to improved stroke care. The Stroke Core Competencies for staff working with people affected by stroke were launched in 2005, and in 2007 the Scottish Government funded a NES/Chest, Heart & Stroke Scotland project to develop an e-learning resource for health and social care staff based on the competencies. The STARs (Stroke Training and Awareness Resources) website was launched in May 2008 and provides an interactive way of learning the stroke competencies. Specialty registrar training in stroke medicine has also been established. Chest, Heart & Stroke Scotland provides stroke training programmes, with funding from NHS Greater Glasgow & Clyde, Lothian, Grampian, Lanarkshire, Fife, Dumfries & Galloway and Borders. These offer in-service training to acute and primary care staff and relevant local authority and other home-care services. The Stroke Research Network funded through the Chief Scientist Office is now very well established, and contributing to national and international trials which will ultimately benefit all those in Scotland who have had a stroke.
2.13 The Chief Medical Officer's annual report Health in Scotland 2007 in its chapter on 'Coronary heart disease and stroke: Reducing amendable mortality', provides a useful summary of recent progress in reductions in the mortality rates of the cardiovascular diseases ( CVD) of Coronary Heart Disease ( CHD) and stroke. It also describes a range of health improvement measures and interventions that have the potential to save up to 10,000 lives from CVD each year in Scotland, if optimally applied.
2.14 This chapter has highlighted key achievements across Scotland since the Strategy was last updated. Chapters 3 and 4 focus on specific areas of heart disease and stroke service delivery which will need particular attention over the next period of the Action Plan, in order to sustain already significant improvements and address areas of relative neglect such as long term care for those who have had a stroke.
There is a problem
Thanks for your feedback