Leading Better Care: Report of the Senior Charge Nurse Review and Clinical Quality Indicators Project
Results of the Senior Charge Nurse Review and Clinical Quality Indicators Project conducted by the Scottish Government and professional advisers.
Section 2
Senior Charge Nurse Review
The aim of the SCN Review was to create a modern clinical leadership role to enable frontline senior charge nurses to maximise their contribution to delivering safe and effective care by developing their leadership capacity and capability. The scope of the review included all nurses and midwives who lead a team that provides care to patients within hospitals.
The review's objectives were to:
- seek stakeholder views on the role and its potential for development
- describe the clinical coordination, leadership and management functions of Senior Charge Nurses
- develop a framework for the SCN role
- provide guidance for NHS boards on developing SCN roles locally (this will be outlined in the Implementation section).
Outcomes of Stakeholder Views of Senior Charge Nurse Role
At the outset of this review we already understood that Senior Charge Nurses have a key role in determining quality of care within wards and departments. However, as health service management structures have changed, SCN roles and responsibilities have become multifaceted and now tend to vary in scope across NHSScotland. For some senior charge nurses, this has meant a shift away from the focus of providing clinical coordination and managing patient care in their areas of clinical responsibility.
The early stages of the project examined how the SCN role was perceived both in the literature and by stakeholders. The key findings of this are outlined in Table 1.
There was consensus among stakeholders that NHSScotland should recognise and value the SCN role. Stakeholders felt that standardisation of the role across NHSScotland, with key responsibilities defined, core competencies described and an exemplar job description and Knowledge and Skills Framework ( KSF) outlines agreed, would be beneficial in this regard.
To complement the stakeholder perspective, an activity analysis of senior charge nurses within development sites was completed. This demonstrated that SCN time was distributed equally between:
- ensuring safe and effective clinical practice
- enhancing patient experience
- managing and developing the performance of the team.
This analysis also found little SCN time spent on explicitly contributing to the delivery of the organisation's objectives. Indeed, the disengagement between the strategic direction of NHS organisations and senior charge nurses as frontline clinical leaders was a key theme that emerged throughout the review process.
Table 1. Perceptions of role of SCN
Source/stakeholders |
Perceptions/findings |
Patients and public |
|
Stakeholder workshops |
|
Survey of SCNs |
|
Learning and development needs analysis of SCNs |
|
Interviews with executive directors and chief executives |
|
Literature review |
|
Literature review |
Influence patient outcomes |
Clinical coordination, leadership and management functions of the Senior Charge Nurse
The outcomes of the stakeholder consultation and activity analysis informed the development of the description of the clinical coordination, leadership and management functions of senior charge nurses. These outcomes are outlined below.
Clinical coordination
From their consideration of the SCN role, stakeholders were able not only to define the elements of the role they believed to be crucial, but also to identify current role components they believed were not essential parts of their function. Stakeholders' concerns over parts of the current role were highlighted by the outcomes of the SCN activity analysis, which demonstrated that a lot of SCN time was spent on general administrative duties, with a small number also providing hospital or directorate cover and a significant number providing direct clinical care to a caseload of patients.
The clinical coordination aspect of the role has generated a great deal of discussion and there is a risk that this may be misunderstood. To define the role of clinical coordination, it may help to identify some of what this does and does not encompass (Table 2).
Leadership
Senior charge nurses across Scotland already have a good platform to continue to build on their leadership skills as 75% of those responding to the SCN survey have been involved in a leadership programme. It is clear from the views gathered from patients and public that they perceive senior charge nurses as having a clear leadership role. They want then to be:
- visible
- identifiable
- accessible
- approachable
- authoritative.
Table 2. Scope of clinical coordination
Aspects of SCN role in clinical coordination |
Not part of SCN role in clinical coordination |
Clinical expert and coordinator for all patients in the ward/area |
Providing care by having a direct clinical case load |
The senior charge nurse has a significant clinical leadership role that includes:
- developing a culture of person-centred care
- leading the delivery of clinically excellent, high-quality services
- ensuring a culture of continuous quality improvement
- influencing and facilitating change.
Management function
Senior charge nurses also carry the functions of manager for their ward/department. These include:
- efficient and effective use of resources
- managing the performance of the team
- planning and monitoring staffing levels to match requirements of workload
- ensuring compliance with local and national standards, policies and legislation.
Framework for SCN Role
The views and consensus from the extensive stakeholder involvement, literature review and the SCN activity analysis were used to inform the development of a framework for the SCN role. The starting point for this was the identification of areas of responsibility:
- to ensure safe and effective clinical practice
- to enhance patient experience
- to manage and develop the performance of the team
- to contribute to the delivery of the organisation's objectives.
The key result areas linking to these four main areas of responsibility are highlighted below (see Figure 2). The details relating to these areas of responsibility are defined in Table 3.
Figure 2. Responsibilities and key result areas of SCN role
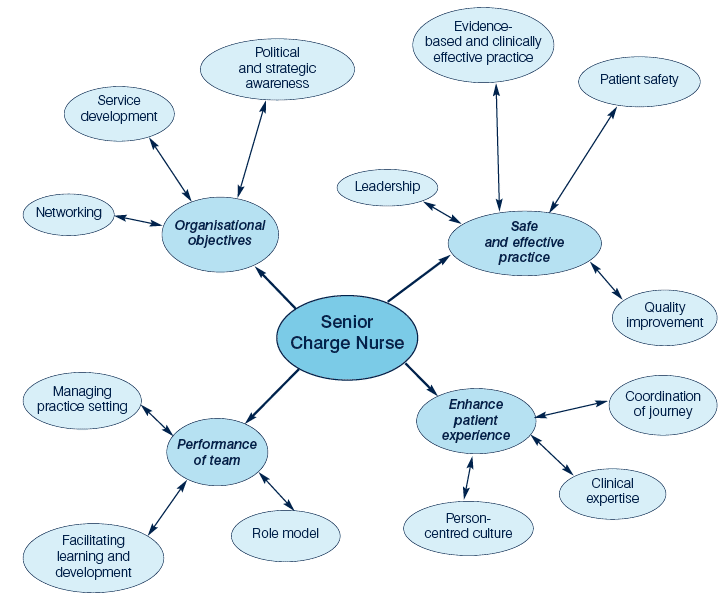
Table 3. Details of SCN Role Framework
1. Ensure safe and effective clinical practice
1.1 Clinical leadership and team working
As clinical leader, promote teamwork within a multiprofessional environment, demonstrating critical analysis and decision-making skills; lead the delivery of a clinically excellent, high-quality service; influence and facilitate change within the ward/department and, where appropriate, the organisation.
1.2 Evidence-based, clinically effective practice
Act as a change agent, lead the development of clinically effective practice through the effective use and integration of evidence; set, implement and monitor evidence-based policies, procedures and protocols.
1.3 Continuous quality improvement
Ensure a culture of continuous quality improvement through the use of audit, patient feedback and reflection on practice by self and other members of the team.
1.4 Patient safety
Promote a clean and safe environment for staff, patients and visitors by ensuring compliance with legislation, policies and protocols, including health and safety, healthcare associated infection, risk management and critical incident reporting and analysis; assess and manage actual and potential risks to health and well-being.
Ensure a high standard of record keeping in accordance with Nursing and Midwifery Council requirements, national legislation and local standards, facilitating effective communication with the multi-professional team regarding patient care.
2. Enhance patients' experiences
2.1 Coordination of the patient journey
Ensure coordination of the patient's journey by planning and coordinating the episode of care, including the smooth transition to other settings, promoting effective discharge and communicating with multidisciplinary and interagency teams as required.
2.2 Clinical expertise
Coordinate nursing/midwifery interventions, influencing clinical decisions and monitoring the quality of patient care provided through using expert clinical knowledge relevant to their own field of practice, underpinned by theory and experience.
2.3 Promote a culture of person-centred care
Within a multidisciplinary team environment, develop a culture of person-centred care; maintain high visiblity within the ward/department; communicate regularly with patients, relatives and/or carers; promote a caring environment where equality and diversity issues are respected and patients are enabled to be partners in their care.
Identify opportunities to develop care and services by ensuring that there are effective systems in place to access patients and carer experience/feedback and ensure complaints are managed in line with organisational policy, including the dissemination of learning points.
3. Manage and develop the performance of the team
3.1 Role modelling
Act as a role model, creating a supportive ethos to empower staff to contribute to the delivery of high-quality, person-centred care.
3.2 Learning and development
Support the learning and development of all staff; create a learning environment that ensures effective learning opportunities for staff and students, including appropriate orientation and induction programmes and a range of clinical support strategies (mentoring, coaching, clinical supervision and action learning) and planning ongoing mandatory training and relevant education/development opportunities.
Support the career pathway of individual team members by ensuring all staff have opportunities for individual performance review and personal development plans and maintain an up-to-date knowledge of current clinical, professional and legal issues.
3.3 Manage the practice setting
Manage the practice setting, ensuring effective use of resources and workforce planning by monitoring workload and, through efficient rostering, maintain appropriate staffing levels and skill mix, taking account of role and competence of staff when delegating work; contribute to the management of the ward/department budget.
Manage the nursing/midwifery team, ensuring compliance by self and others with professional standards, legislation, national and organisational policies; leading recruitment, selection and attendance management initiatives; ensure grievance and disciplinary matters within own department are identified, actioned and reported to the appropriate manager.
4. Contribute to the delivery of the organisation's objectives
4.1 Networking
Network with peers across professional groups, promoting the exchange of knowledge, skills and resources.
4.2 Service development
Work in partnership with a range of clinicians and managers in the planning or development of own service, promoting the involvement of patients and the public.
4.3 Political and strategic awareness
Develop and maintain a working knowledge of local, national and professional strategy and policy; ensure that organisational goals are reflected in personal objectives and in ward/department development plans and demonstrate the ability to contribute to policy and strategy development at departmental and organisational levels and, where appropriate, national level.
Table 4 demonstrates how the four key functions within the Framework for the SCN link with the Knowledge and Skills Framework.
Table 4. Links to Knowledge and Skills Framework of the four dimensions of the SCN Role
Framework for the Senior Charge Nurse Role |
NHSKSF |
1. Ensure safe and effective clinical practice |
1.1 Core 1, Core 4, Core 5 |
2. Enhancing patients' experiences |
2.1 Core 1, HWB2 |
3. Manage and developing team performance |
3.1 Core 2, Core 5 |
4. Contribute to the delivery of the organisation's objectives |
4.1 Core 1, Core 4 |
The publication of the Education and Development Framework for Senior Charge Nurses ( NHS Education for Scotland, 2008) will equip senior charge nurses with a tool to guide and support them in their development journey. This can be accessed at www.nes.scot.uk .
Summary of SCN Review
Senior charge nurses have an important role in providing clinical leadership to their teams to ensure that patients in their wards/departments receive high-quality care. This is not just about how they perform as individuals, but also how their teams are developed. The framework developed during the course of the SCN Review, which is outlined in detail above, will contribute to ensuring that there is a consistent approach to the role across NHSScotland.
Senior charge nurses across NHSScotland are motivated to continue to build on the quality of care and experience for patients in their areas of responsibility. The SCN Review will assure senior charge nurses that they are valued in this role and that their significant contribution to health care is recognised. This focus on quality is also supported by the results of the CQI project.
There is a problem
Thanks for your feedback